SPINAL MUSCULAR ATROPHY
DAVID J. ABRAHAM, M.D. Resident, Orthopaedic Surgery
J. RICHARD BOWEN, M.D. Chief Department of Orthopaedic Surgery
ALFRED I. DUPONT INSTITUTE
April 16, 1996
CASE HISTORY:
Kg is a 6+6 year old white female evaluated in the orthopaedic clinic
for progressive scoliosis, bilateral hip dislocations and diffuse hypotonia
with inability to walk.
Past medical history significant for recurrent upper respiratory infections
occasionally requiring hospitalization.
Developmental History: 8 pound 6 ounce, full term female with no perinatal
events and normal intrauterine movement was developing normally until 6
months of age when parents noticed she stopped moving her legs and lost
the ability to roll over.
Pediatric neurologist diagnosed Spinal Muscular Atrophy after reviewing
the muscle Biopsy.
Managed with physical therapy and inpatient rehabilitation consisting
of intensive physical, occupational and aquatic therapy and the use of
long leg braces at age of 2.
Radiographic evaluation at age of 3 showed mild scoliosis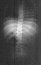 and bilateral dislocated hips.
and bilateral dislocated hips.
Parents were informed that scoliosis would likely progress and PSF would
be needed in the future.
Age 6 scoliosis progressed to 78 degrees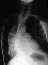 and PSF with the unit rod
and PSF with the unit rod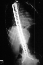 was performed.
was performed.
DISCUSSION :
A group of disorders characterized by degeneration of the anterior horn
cells of the spinal cord and occasionally the neurons of the lower bulbar
motor nuclei resulting in muscle weakness and atrophy.
Autosomal recessive disorder that occurs in one in 20,000 live births.
One in 40 to 80 people are carriers of the gene.
Loss of the anterior horn cell is acute event without neurologic progression.
The progression of muscle weakness is a reflection of normal growth
that exceeds muscle reserve.
Respiratory function is compromised causing atelectasis and pneumonia
and eventually resulting in death .
CLINICAL CLASSIFICATION:
Based on age of onset and functional capacity at time of presentation
.
- Type I: Acute Werdnig Hoffman Disease
- Clinical onset is from birth to 6 months
- Typically have severe involvement with weakness and severe hypotonia
- No head control, will never roll over or sit unassisted
- Usually die secondary to respiratory failure before age 2
- Type II: Chronic Werdnig Hoffman Disease
- Onset from 6 months to 24 months of age
- Less involved than Type I, will sit, but will never walk
- May live 30 to 40 years
- Type III: Kugelberg-Welander Disease
- Onset from 2 to 10 years of age
- Usually walk until late childhood or early adolescence, never run
- + Gower sign secondary to proximal muscle weakness with pseudohypertrophy
of claves
CLINICAL FEATURES:
- Symmetric limb and trunk weakness with muscle atrophy greater in the
lower extremities than the upper extremities; and greater atrophy in the
proximal muscle groups than the distal muscle groups.
- Hypotonia and areflexia
- Sensation and intelligence are normal.
- Diffuse muscle involvement involves all muscles except diaphram, sternohyoid,
sternothyroid and involuntary muscles of heart, bladder, intestine, and
sphincters.
DIAGNOSTIC STUDIES:
- Labs: usually normal
- EMG/NCS: Fibrillation potentials associated with denervation are the
best diagnostic signs
- Muscle Biopsy: Loss of fibers and atrophy within normal groups of fiber
bundles
No evidence of primary myopathy
TREATMENT:
Orthopaedic concerns involve the treatment of soft tissue contractures
of the lower extremities, hip subluxation or dislocation and inevitable
spinal deformity.
- Soft tissue contracture:
- Results from progressive muscle degeneration and replacement with fibrous
tissue
- Ambulation preserved by orthoses
- Worsens quickly after pt is confined to wheelchair
- Hip subluxation/dislocation
- Treatment may preserves sitting balance, pelvic alignment and increase
comfort
- Some authors recommend treatment of dislocated hips however the redislocation
rate has proven to be significant due to the progressive degeneration of
the proximal muscles (8)
- Others recommend symptomatic treatment of dislocated hips ie, adductor
tenotomy for contracture
- Spinal Deformity
- 100% of type II, and most of Type III develop scoliosis with resulting
decrease in pulmonary function
- Typically begins in the first decade of life, is progressive and resistant
to bracing
- Bracing may slow the progression to delay fusion until adolescence
(2)
- Surgery indicated for
1. Curve greater than 40 degrees
2. FVC less than 40 % of normal
- Schwentker (7) reviewed nine patients with SMA treated with PSF and
concluded that 8 of 9 lost function but 7 of 9 stated gains in comfort
and spinal stability outweighed functional loss
- Aprin and Bowen (1) reviewed 22 patients with SMA who underwent spine
fusion and concluded that:
1. Long posterior fusion was the best way to prevent secondary curves
above and below the fusion
2. Anterior arthrodesis alone was not sufficient to maintain spinal
stability
3. Anterior arthrodesis was associated with significant increase in
pulmonary complications
4. Pre and post operative PT were essential to preserve function.
5. Spine arthrodesis reduced the rate of pulmonary deterioration but
did not prevent its progression
- Granata (6) reviewed the natural history of spinal deformity in SMA
and concluded that scoliosis is inevitable and progressive in nonambulatory
patients and rarely becomes significant in ambulatory patients
- Furumasu (5) reviewed 40 pateints after PSF and showed that fusion
caused a significant decrease in gross motor funcion and an increase in
the use of upper extremity assistance devices
- Brown (3) noted that PSF patients never attain thair preoperative functional
levels
Recommendation: Presently we recommend posterior spinal arthrodesis
with segmental fixation from T1 to the pelvis and currently use the Unit
Rod System.
REFERENCES:
- Aprin H, Bowen JR, MacEwen GD, Hall JE. Spine arthrodesis in patients
with spinal muscular atrophy. J Bone Joint Surg A-64, 1982, 1179.
- Bowen JR, Forlin E. Spinal muscular atrophy. In: Weinstein SL, ed.
The pediatric spine. Principles and practice. New York: Raven Press, 1994:1025.
- Brown CJ, Zeller JL, Swank SM, it al. Surgical and functional results
of spine fusion in spinal muscular atrophy. Spine 1989; 14: 763.
- Daher YH, Lonstein JE, Winter RB, Bradford DS. Spinal surgery in spinal
muscular atrophy. JPO 1985; 5: 391.
- Furumasu J, Swank SM, Brown JC, et al. Functional activities in spinal
muscular atrophy patients after spinal fusion. Spine 1989; 14: 771.
- Granata C, Merlini L, Magni E, et al. Spinal muscular atrophy. Natural
history and orthopaedic treatment of scoliosis. Spine 1989; 14:760.
- Schwentker EP, Gibson DA. The orthopaedic aspects of spinal muscular
atrophy. JBJS 1976; 58, 32.
- Thompson CE, Larsen LF. Recurrent hip dislocation in immediate spinal
atrophy. JPO 1990; 10: 638.
![]() and bilateral dislocated hips.
and bilateral dislocated hips. ![]() and PSF with the unit rod
and PSF with the unit rod![]() was performed.
was performed.