 who also had excellent re-modeling 3.5 year later.
who also had excellent re-modeling 3.5 year later. THE ALFRED I. DUPONT INSTITUTE
WILMINGTON, DELAWARE
During 1989 through 1991, 50 children with spastic cerebral palsy were operated on by the senior author using varus and pelvic osteotomy procedure. The majority (88%) of these children were non- ambulatory with spastic quadriplegic pattern involvement. The remaining 6 children were diplegic involved with some degree of ambulatory ability.
From January 1989 to November 1991, 50 children with 42 subluxated and 27 dislocated hips under went reconstruction using the above protocol. Of these 69 hips, 58 had a combination pelvic and femoral osteotomy and 11 hips had only a femoral osteotomy. In addition 26 femoral osteotomies were done to provide for symmetry of the lower extremities. In addition, 49 dysplastic hips had adductor muscle lengthening. Only (6) of the dislocated hips required a medial capsulectomy to allow for reduction into
the acetabulum. Every patient in this group had a pelvic otseotomy and 8 children had bilateral pelvic osteotomies. The mean operative time was 3 hours 20 minutes with a mean blood loss of 17.6 ml per kg or 387 cc per patient. This group of patients included 18 patients with previous adductor tenotomy and neurectomy, 8 patients had had previous varus femoral osteotomy (5 bilateral, 3 unilateral), 3 had prior posterior spine fusion and one had a prior dorsal rhizotomy. Reduction and stability of the hip defined as MP less than 30 has been maintained in 94% of the 69 hips with greater than two year follow up.
Prior to reconstruction, 23 hips in 18 patients were painful (5 bilateral and 13 unilateral). At final follow- up of over 2 years, 1 hip remained painful requiring reconstructive surgery with prosthetic replacement 9 months after reconstruction, 3 hips continued with some pain although improved and not enough to warrant further surgery at this time, therefore there was 82 percent complete removal of the pain, 14% improved in pain but not complete resolution, and 4% failure of pain relieve.
Hip range of motion has increased from a mean 16 degrees pre- operatively to 30 degrees post- operatively. Since the original surgery, 6 hips in six patients have required repeat adductor release and one patient developed a significant restriction of hip motion secondary to severe heterotopic bone
formation requiring resection. Her range of motion was limited to minus 45 degree extension, 80 degrees of flexion, no rotation, zero adduction, and 20 degrees of abduction. This was the only patient with heterotopic bone formation which restricted hip range of motion. She was also the only patient to have this procedure less than 3 months following spine fusion. This procedure was done 10 days after spine fusion.
The mean MP for dislocated hips pre- operatively was 94% and those with
full follow- up excluding the 2 dislocated hips was 13%. Subluxated hips
had a pre- op mean of 51% and at follow- up were at 7%. The mean pre- op
MP for hip treated with pelvic and femoral osteotomy was 73% and at follow-
up was 7%. For those hips with only a varus osteotomy a pre- op 43% was
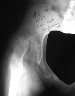
noted and at follow- up were 12 %. The radiographic outcome is generally
excellent as demonstrated by the outcome of this painful dislocated 8 year
old ![]() who on 4.5 year follow up had a normal hip especially notice the excellent
development of the lateral aspect of the acetabulum.
who on 4.5 year follow up had a normal hip especially notice the excellent
development of the lateral aspect of the acetabulum. ![]() Also the ability to remodel as a teenager is shown by this very hip in
a 16 year old
Also the ability to remodel as a teenager is shown by this very hip in
a 16 year old  who also had excellent re-modeling 3.5 year later.
who also had excellent re-modeling 3.5 year later. ![]() Another example is this boy who was a household ambulator until he developed
severe pain from hip subluxation
Another example is this boy who was a household ambulator until he developed
severe pain from hip subluxation ![]() and 3 years after reconstruction he is pain free and again an independent
community ambulator.
and 3 years after reconstruction he is pain free and again an independent
community ambulator. ![]()
These questionnaires were answered by the parent or principle care taker with 38 questionnaires being completed. Two parents refused to participate and 10 parents or caretakers who knew the child both pre-op and post-op could not be found. From a pre- op review of complaints, 27 patients (54%) presented with perineal hygiene problems, and 22 patients had significant problems with seating. On the follow up questionnaire only one parent complained of perineal care problems and 1 noted that sitting ease and comfort was worse while 7/37 were no change and 29/37 had improved ability to sit or were more comfortable sitting. The child's ability to stand, head control, eating, and feeding were largely unaffected by the procedure. Parents were ask if they would recommend the surgery to another parent and 32/37 (86%) said yes, 3/37 were unsure, and 2/37 said no.
The best treatment for spastic hip subluxation and dislocation is prevention by early recognition and muscle balancing surgery, however some patients will fail this treatment and in our practice we still see a large number of patients who are not receiving preventive care and present with painful dislocations. This type of reconstruction which addresses all of the deformity provides for better intermediate term stability and function of the hips. Utilizing this procedure we were able to normalize 95% of hips on follow- up. There were, however two repeat dislocations, both of which were due to very severe direct posterior acetabular insufficiency and internal rotation, adduction contracture of the hip. This problem requires further investigation since repeat attempt in one hip resulted in repeat dislocation and the reconstruction in the second patient is still not of sufficient follow- up to comment on its merit. Careful close post-operative follow-up is indicated with repeat soft tissue release if significant contractures are reoccurring. A cause of the internal rotation contracture which was found on case 5 was the anterior gluteus medias and gluteus mimimus. These muscle are not generally considered to be internal rotators however after the varus osteotomy their mechanical advantage is increased apparently as was demonstrated by the dramatic improvement in external rotation after their release.
The major problem of the continued subluxated hip, although mild appears most related to not doing acetabular reconstruction in two of the three subluxed hips. There were no complication directly related to the pelvic osteotomy and it's addition provided an improved acetabular coverage, therefore it is difficult to justify taking the chance of a poorer outcome. Also 8 of the previously failed varus osteotomies only all had type 2 sourcils meaning they were sloping laterally above the horizontal at the time of the initial varus osteotomy. Also both of the subluxated hips on final follow-up which had only a varus osteotomy had a type 2 sourcil.
The other major goal of this procedure was to develop a method which would allow immediate mobilization of these compromised patients which should allow them to return to school earlier, and make home care easier . In those patients which were treated without a cast there were only two fractures out of 50 patients for 4% while Mubarak reported 1 fracture in 11 patients for 10%, Sturm reported 6 of 21 for 29% incidence and Pritchett reported 18% incidence. This strongly suggests that the goal of immediate mobilization does reduce post-op fracture incidence. It is more difficult to document other positive changes however all six parents who had previously cared for the same child in a cast much preferred the immediate mobilization without a cast. It is the general impression of floor nurses that the first 48 to 72 hours, the child is more uncomfortable and more difficult to handle than when a cast is used.
[Orthopaedic Department Home Page, Cerebral Palsy Home Page, Gait Lab Home Page, Top (Spastic Hip Outcome)]