 .
There was a healing transverse subtrochanteric fracture involving the lateral
cortex
.
There was a healing transverse subtrochanteric fracture involving the lateral
cortex 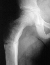 .
There was also an expansile lesion noted in the midshaft of the right fibula
.
There was also an expansile lesion noted in the midshaft of the right fibula
DOUG ALBRACHT, D.O. Resident, Orthopaedic Surgery
WILLIAM MACKENZIE, M.D., Attending Pediatric Orthopaedic Surgeon
June 19, 1996
CLINICAL CASE PRESENTATION
ORTHOPAEDIC DEPARTMENT
THE ALFRED I. DUPONT INSTITUTE
WILMINGTON, DELAWARE
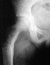
A 10 year old white female was evaluated in the orthopaedic clinic for leg length discrepancy. This child was diagnosed with McCune-Albright's Syndrome at the age of 6 years. Her disease process has been characterized by early breast development at 3 years of age, menarche at the age of 6, and a pathologic subtrochanteric fracture after a trivial fall at age 8. She now complains of a limp and pain after long walks. She is undergoing a medical treatment protocol at NIH related to the precocious puberty.
The patient demonstrated a large pigmented lesion with irregular border
located in the right upper back. There was a two centimeter leg length
discrepancy by the block test. X-rays showed an expansile radiolucent area
with a ground glass density involving the right proximal femur  .
There was a healing transverse subtrochanteric fracture involving the lateral
cortex
.
There was a healing transverse subtrochanteric fracture involving the lateral
cortex  .
There was also an expansile lesion noted in the midshaft of the right fibula
.
There was also an expansile lesion noted in the midshaft of the right fibula
![]() .
A scanogram revealed a 1. 8 cm leg length discrepancy with right leg shorter
than left
.
A scanogram revealed a 1. 8 cm leg length discrepancy with right leg shorter
than left ![]() .
Bone age was 14 years old ( 4 years advanced)
.
Bone age was 14 years old ( 4 years advanced) ![]() .
.
Fibrous dysplasia is an intramedullary diaphyseal /metaphyseal lesion that blends with a thinned, slightly bulged cortex. The cortex of the affected bone may be thinned by endosteal erosion which creates a scalloped pattern. In long bones, the lesions are usually metaphyseal in location, extending into the rnid-diaphysis. The lesion has a homogenesis density @g it a so-called "ground glass" appearance. An angular deformity in the bone is often present at the level of the lesion. Periosteal reaction is absent except when a pathologic fracture is present. Bone scans show increased uptake-can assess the extent and multiplicity of involvement. CT scan is helpful in differentiating eosinophilic granuloma, osteomyelitis, and unicameral bone cyst. These show lower Hounsfield units (O to 40), compared to fibrous dysplasia (70 to 130). Few studies other than plain X-rays are required in a typical case of polyostotic disease.
Fibrous dysplasia is composed of fibrous stroma with normal appearing nuclei and irregular shaped strands of osteoid and bone. There are few if any osteoblasts, the osteoid and bone seem to arise directly from the background of fibrous stroma. The bone is organized irregularly, and often shaped like the letter "C" or "O".
In children, skeletal lesions are likely to progress. There may be extension of existing lesions and the involved bones may show increasing deformity. New lesions may appear in areas that were previously normal. Following maturity, the lesions tend to be stabilized in respect to growth, but they still have woven trabecular bone not lamellar bone patterns. The lesions do not become sclerotic and there is no concentration of trabeculae along stress lines. Healing occurs with periosteal callus usually within a normal time frame. Delayed union or nonunion are very rare. Progressive deformity may be produced by malunion of specific fractures or gradual "bending" of the bone due to subclinical chronic insufficiency fractures.