KYPHOSCOLIOSIS AND NEUROFIBROMATOSIS
MARTIN JENTER, D.O., Orthopaedic Resident
KIRK DABNEY, M.D., Attending Pediatric Orthopaedic Surgeon
January 31, 1996
CLINICAL CASE PRESENTATION
ORTHOPAEDIC DEPARTMENT
THE ALFRED I. DUPONT INSTITUTE
WILMINGTON, DELAWARE
CASE HISTORY:
- HISTORY: This male child was diagnosed at age 3 with Neurofibromatosis
type 1. At the age of eleven years old he presented to the Institute with
a complaint of thoracic back pain (1991) after two years of observation
of a thoracic scoliosis.
- PHYSICAL EXAM: His presentation includes multiple cafe-au-lait spots
larger than 1.5 cm and Lisch nodules and his mother is diagnosed with Neurofibromatosis
type 1.
- XRAYS: At his first visit the patient was diagnosed with a kyphoscoliosis
that measured 62 degrees of a right thoracic T3-T7 curve
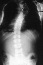 and a 62 degree thoracic kyphosis
and a 62 degree thoracic kyphosis .
His initial X-rays revealed posterior body scalloping and enlarged foramina
consistent with neurofibromatosis . The patient had no known illnesses,
showed no evidence of developmental delay and was active in school sports.
He denied any neurologic symptoms.
.
His initial X-rays revealed posterior body scalloping and enlarged foramina
consistent with neurofibromatosis . The patient had no known illnesses,
showed no evidence of developmental delay and was active in school sports.
He denied any neurologic symptoms.
- TREATMENT:
- FOLLOW-UP:
Physical Findings:
Significant findings are the cafe-au-lait spots on torso and extremities,
axillary and inguinal freckling, plexiform neuroma right flank, obvious
kyphosis and scoliosis with shortened trunk in relation to extremities,
ligamentous laxity of fingers and elbow. Gait, reflexes and neuromuscular
exam are all normal.
Treatment:
In preparation for spinal fusion for stabilization of this kyphoscoliosis
he underwent a MRI of the brain cervical and thoracic spine and CT of the
thorax. The brain and cervical spine showed no evidence of tumor. The lower
cervical and upper thoracic canal was enlarged without evidence of cord
compression, a finding consistent with dural ectasia 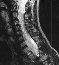 .
There is soft tissue protrusion into the thoracic canal that may resemble
a dumbbell lesion.
.
There is soft tissue protrusion into the thoracic canal that may resemble
a dumbbell lesion.
Coinciding with current literature recommendations for treatment of
severe dysplastic kyphoscoliosis, the patient underwent an Anterior-Posterior
spinal fusion from T1-T10. The scoliosis was corrected to 21 degrees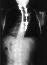 and kyphosis to 34 degrees. The procedure was augmented with a rib strut
graft and was tolerated well. No neurologic complications occurred and
the patient developed a solid fusion by one year without progression of
the curvature. He is currently 5 years post-op playing in sports and without
pain.
and kyphosis to 34 degrees. The procedure was augmented with a rib strut
graft and was tolerated well. No neurologic complications occurred and
the patient developed a solid fusion by one year without progression of
the curvature. He is currently 5 years post-op playing in sports and without
pain.
SCOLIOSIS AND NEUROFIBROMATOSIS
Incidence:
Most common skeletal problem in NF is scoliosis. Occurs in 3% of patients
with scoliosis that are seen in a scoliosis clinic and 60% of all patients
seen in a neurofibromatosis clinic.
Types:
Dysplastic: Short-segmented, sharp angled scoliosis with severe wedging
of the apical vertebrae. Foraminal enlargement, scalloping vertebrae, pencil-like
ribs, spindling transverse process and apical rotation all signs of dysplasia.
Ribs may protrude into canal. Progressive, no standard pattern.
Nondysplastic: Resembles idiopathic scoliosis with equal right and left
thoracic curves. Progression of
curves with or without fusion is faster than idiopathic.
Cause:
Exact cause is unknown but believed to be secondary to either osteomalacia,
local fibromas, endocrine abnormality or mesoderm dysplasia.
Kyphosis:
Considered pathologic if greater than 49 degrees. Possibly secondary
to collapse of apical dystrophic vertebrae with flexion force created by
rotation with the scoliosis. Kyphosis contributes more to paraplegia as
a result of tension on cord with flexion. This typically occurs in the
upper thoracic region where the cord -canal ratio is most critical.
Management:
All patients going to surgery or undergoing spinal manipulation need
cervical X-rays. If dystrophic changes on AP or Lat do obliques to look
for dumbbell lesion and flex/ext for instability. MRI or CT myelogram to
evaluate for intra or extradural mass, menigeocele, dural ectasia.
Cervical Treatment:
Posterior spinal fusion for severe deformity and instability. Autologous
graft and halo. If previous laminectomy, do anterior and posterior fusion.
Thoracic Scoliosis:
Dystrophic type:
- Bracing is ineffective.
- If kyphosis less than 49 degrees, consider posterior fusion with instrumentation.
- For increased kyphosis or scoliosis greater than 40 degrees, consider
anterior-posterior fusion with anterior strut grafting with rib, fibula,
iliac crest or tibia and posterior instrumentation. Graft concave side.
- Curves less than 20 degrees observe every 6 months.
- Curves from 20-40 degrees scoliosis consider posterior fusion and instrumentation.
Fusion from neutral vertebrae above and below curve. Post-op immobilization
with Risser cast or TLSO recommended up to one year or until fusion complete.
Laminectomy alone is not recommended . Does not eliminate neurological
symptoms and results in worsening kyphosis.
Nondystrophic type:
- Treat like idiopathic scoliosis.
- Observe curves less than 20 degrees
- Brace from 20 to 35 degrees.
- Consider posterior spinal fusion with instrumentation for curves 35
to 60 degrees
- Consider posterior spinal fusion and ant-posterior with instrumentation
for curves > 60 degrees
RESULTS:
Nondystrophic curves:
- 13% pseudoarthrosis rate by Crawford. Tendency of nondystrophic to
become dystrophic curves.
Dystrophic curves:
- Kyphoscoliosis, curve > 50 degrees, pseudoarthrosis 64% with Winter
for posterior fusion with and without instrumentation (7/11 pts. failed
initial treatment). With A-Post. fusion Winter had 5/8 solid union(65%).
- Calvert had 12/15 fusions with posterior instrumentation for kyphosis
avg. 50 degrees. Ant.-post. fusion done with avg. kyphosis 110 and scoliosis
96 degrees had 3/4 solid fusions( 75% success).
REFERENCES:
- Calvert, P.T., Edgar, M.A., Webb, . Scoliosis in Neurofibromatosis.
JBJS(Br) 1989;71-B:246-51.
- Chaglassian, J.H., Riseborough, E.J., Hall, J.E. Neurofibromatous Scoliosis.
JBJS 1976;58-A:695-702.
- Crawford, Alvin. Pitfalls of Spinal Deformities Associated with Neurofibromatosis
in Children. Clin Orthopedics and Related Research 1989;245: 29-41.
- Crawford, Alvin. Neurofibromatosis. The Pediatric Spine: Principles
and Practice. 1994;ch 28: 619- 649.
- Winter, R.B., Moe, J.H., Bradford, D.S., Lonstein, J.E., Pedras, C.V.,
Weber, A.H. Spine Deformity in Neurofibromatosis. JBJS 1979;61-A: 677-694.
 .
There is soft tissue protrusion into the thoracic canal that may resemble
a dumbbell lesion.
.
There is soft tissue protrusion into the thoracic canal that may resemble
a dumbbell lesion. ![]() and kyphosis to 34 degrees. The procedure was augmented with a rib strut
graft and was tolerated well. No neurologic complications occurred and
the patient developed a solid fusion by one year without progression of
the curvature. He is currently 5 years post-op playing in sports and without
pain.
and kyphosis to 34 degrees. The procedure was augmented with a rib strut
graft and was tolerated well. No neurologic complications occurred and
the patient developed a solid fusion by one year without progression of
the curvature. He is currently 5 years post-op playing in sports and without
pain.