LATERAL CONDYLE FRACTURE THROUGH THE CAPITELLUM IN
A CHILD
THOM BROWN, M.D., Resident, Orthopaedic Surgery
WILLIAM MACKENZIE, M.D., Attending, Pediatric Orthopaedic Surgery
November 15, 1995
CLINICAL CASE PRESENTATION
ORTHOPAEDIC DEPARTMENT
THE ALFRED I. DUPONT INSTITUTE
WILMINGTON, DELAWARE
CASE HISTORY:
- HISTORY: Five and 5/12 year old white male sustained a fall onto his
outstretched right arm with immediate complaints of pain and swelling in
his right elbow with an inability to move the arm secondary to pain.
- PHYSICAL EXAM: Physical examination revealed swelling, tenderness and
crepitus over the lateral aspect of the elbow. The skin was intact and
neurovascular examination of the right upper extremity was without deficits.
- XRAYS: Radiographic examination of the right upper extremity revealed
a displaced fracture involving the lateral condylar physis exiting through
the substance of the capitellum.
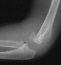
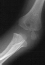
- TREATMENT: The patient was taken to the operating room where under
general anesthesia and tourniquet control the fracture was exposed utilizing
an anterolateral approach, taking care not to disturb the posterior vascular
pedicle of the lateral condyle. Following adequate reduction of the fracture,
2 diverging k-wires were placed across the fracture site.
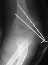
 The
patient was immobilized in a long arm cast at 90 degrees until radiographic
evidence of healing was apparent. The long arm cast and k-wires were removed
in clinic.
The
patient was immobilized in a long arm cast at 90 degrees until radiographic
evidence of healing was apparent. The long arm cast and k-wires were removed
in clinic.
ETIOLOGY
17% of all pediatric elbow fractures.
More common in summer months 5-10 years of age (2-14)
Mechanism: varus stress to an extended elbow with supinated forearm
CLASSIFICATION
ANATOMIC: (Milch)
- Milch I- Fracture extends through the ossification center and exits
at the radiocapitellar groove. The lateral crista is intact, decreasing
the likelihood of elbow dislocation. (Salter-Harris IV)
- Milch II- Fracture line follows the physis completely medially, exitin-
through the trochlear notch rendering the humero-ulnar joint unstable.
(Salter-Harris II)
DISPLACEMENT: (Rutherford)
- Stage I- minimal displacement with intact articular surface
- Stage II- rotation of the fragment with disruption of the articular
surface
- Stage III- fragment is rotated and displaced
DISPLACEMENT RISK: (Finnbogason)
- Fracture line can not be followed to the epiphyseal cartilage (0/65
displaced)
- Fracture line clearly exits through epiphyseal cartilage (6/35 displaced)
- Fracture gap equal medially and laterally (5/12 displaced)
TREATMENT
- Nondisplaced (stage I): posterior splint vs. long arm cast at 90 degrees
flexion with supinated forearm. CLOSE FOLLOW-UP IMPORTANT because of high
incidence of late displacement and eventual non\malunion.
- Displaced (stage II/III): closed reduction and percutaneous pinning
if reducible closed. If not, ORIF with percutaneous pinning, recommended.
Post-operative Management: Long ann cast at 90 degrees until radiographic
signs of healing are evident.
COMPLICATIONS
- Cubitus Varus: Secondary to matunion or capitellar overgrowth. No rotation
as in supracondylar fractures. The deformity is in the coronal plane only,
and usually does not require treatment.
- Fishtail Deformity: Secondary to a break between the ossific nucleii
of the capitellum and trochlea resulting in disruption of the lateral trochlear
epiphyseal vessel, resulting in a deficient lateral lip of the trochlea.
This is also treated conservatively.
- Cubitus Valgus: Secondary to non-union and proximal migration of the
fragment with subsequent elbow instability and eventual tardy ulnar nerve
palsy (20+ years). Cubitus valgus secondary to physeal closure has rarely
been reported. Treatment- transposition +\- osteotomy with ORIF, only if
symptomatic or unstable.
- Late Appearing Fractures: Undiagnosed/untreated fractures >6 weeks
post-injury. Some studies suggest a conservative approach because of the
high risk of capitellar AVN and stiffness secondary to the wide surgical
exposure. Flynn has reported good results utilizing a limited exposure
with pin and bone pe- fixation for slightly displaced fractures.
CONCLUSIONS
- Fractures of the lateral condylar physis that exit through the capitellum
should be treated with the same indications as a Milch II fracture with
emphasis placed on achieving and maintaining articular congruity until
healed by closed or more often open means.
- The length of time to maintain internal fixation and casting should
be dictated by the radiographic appearance of the healing fracture more
so than the length of time of immobilization. Displacement with has been
reported between 3 and 4 weeks post fracture.
REFERENCES
- Dhillon, K.S., et al., Delayed Management of the Lateral Condyle in
Children. Acta Orth. Scand. 1988; 59(4), 419-424.
- Finnbogason, T., et al., Nondisplaced and Minimally Displaced Fractures
of the Lateral Humeral Condyle in Children: A Prospective Radiographic
Investigation of Fracture Stability. JPO,1995; 15, 422-425.
- Flynn, J., Nonunion of Slightly Displaced Fracture of the Lateral Humeral
Condyle in Children: An Update. JPO, 1989; 9,691-696.
- Flynn, J, and Richards J., Nonunion of Minimally Displaced Fractures
of the Lateral Condyle of the Humerus in Children. JBJS, 1971, 53A No.
6, 1096-1 101.
- Jakob, R. et al., Observations Concerning Fractures of the Lateral
Humeral Condyle in Children. JBJS 57B No. 4,430-436.
- Masada, K, et al., Osteosynthesis for Old Established Non-Union of
the Lateral Condyle of the Humerus. JBJS, 1990, 72A, -)2-40.
- Marzo, J., et al., Usefulness and Accuracy of Arthrocraphy in Manacement
of Lateral Humeral Condyle Fractures in Children. JPO, 1990, 10, 317-32
1.
- Milch, H., Fractures and Fracture-Dislocations of the Humeral Condyles.
J. Trauma, 1964, 4, 592-607
- .Roye, D., et al., Late Sur-ical Treatment of Lateral Condylar Fractures
in Children. JPO, 1991, 11, 195-199.
- Rutherford, A., Fractures of the Lateral Humeral Condyle in Children.
JBJS, 1985, 67A No. 6, 851-856.
- Wilkins, K., Operative Management of Upper Extremity Fractures in Children.
American Academy of Orthopaedic Surgeons Monograph Series. 1994, 66-70

 The
patient was immobilized in a long arm cast at 90 degrees until radiographic
evidence of healing was apparent. The long arm cast and k-wires were removed
in clinic.
The
patient was immobilized in a long arm cast at 90 degrees until radiographic
evidence of healing was apparent. The long arm cast and k-wires were removed
in clinic. 
 The
patient was immobilized in a long arm cast at 90 degrees until radiographic
evidence of healing was apparent. The long arm cast and k-wires were removed
in clinic.
The
patient was immobilized in a long arm cast at 90 degrees until radiographic
evidence of healing was apparent. The long arm cast and k-wires were removed
in clinic.